






 How is carpal tunnel syndrome diagnosed?
How is carpal tunnel syndrome diagnosed?
History -The doctor often suspects CTS from the patient's history
and symptoms. If the patient complains of numbness and tingling in the
thumb and fingers (supplied by the median nerve) the doctor suspects CTS.
If symptoms worsen with the typically suspected activities (such as driving,
writing, reading, or combing hair) or the patient's work and activity
patterns involve repetitive motions, the doctor will suspect CTS.
Examination - The doctor will determine if there is decreased feeling
in the thumb, index finger, long finger, and ring finger. In severe cases,
the doctor may find that the muscles of the thumb have atrophied (become
smaller).
Testing - The doctor may do some manual tests to confirm the diagnosis
of CTS.
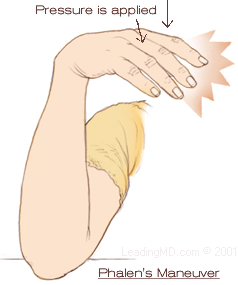
Phalen's Maneuver - The patient
holds the wrist in a bent position for one minute. If CTS is present,
the added pressure on the nerve will make the numbness worse.
Tinel's Sign - The doctor will
gently tap on the wrist where the median nerve travels through the tunnel.
Patients with CTS experience a feeling of electricity or tingling, similar
to the sensation that occurs when the "funny bone" is bumped.
Electrodiagnostic Studies
- Physicians who specialize in nerve function often use more objective
techniques to confirm CTS and evaluate the severity of nerve damage. These
tests are not essential to make a diagnosis of carpal tunnel syndrome, but
they are very helpful in ruling out other problems like pinched nerves in
the neck or arm.
A nerve conduction study is
performed by applying a very mild electrical current along the path of
the nerve. The speed the current travels along the nerve indicates how
well the nerve is working.
Electromyography measures
the electrical activity of muscles. Extremely small, threadlike needles
are placed in certain muscles. Any deviation from normal muscle activity
indicates a problem with the nerve supply to that muscle.


© 2016 by LeadingMD.com All rights reserved.
Disclaimer







 How is carpal tunnel syndrome diagnosed?
How is carpal tunnel syndrome diagnosed?